Partners in Health study highlights need for life-saving medical oxygen
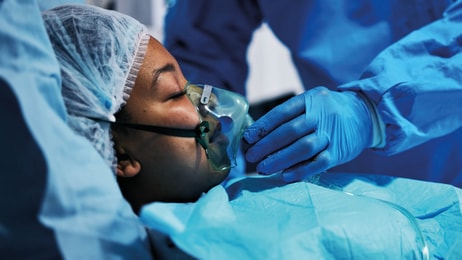
A case study undertaken by social justice organisation Partners In Health (PIH) has revealed the importance of increasing the supply of medical grade oxygen in low and middle income countries (LMICs) to treat diseases such as Covid-19, TB, and other chronic conditions.
Although most developed nations have little to worry about when it comes to supply of medical oxygen, developing countries are still lacking in medical grade oxygen supply and its associated delivery equipment.
According to PIH, even prior to the heightened demand for oxygen during the Covid-19 pandemic only 10% of hospitals in LMICs had access to pulse oximetry and oxygen therapy. Even then, just 20% of the patients who needed life-saving oxygen actually received it.
... to continue reading you must be subscribed